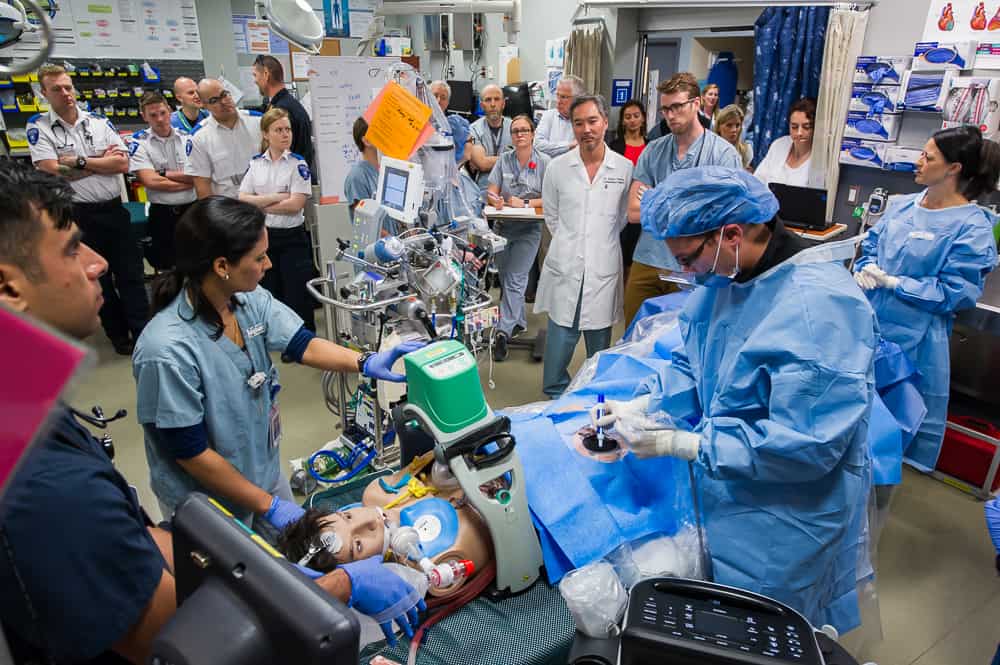
Physicians at St. Paul’s want to start a unified simulation program for PHC
“No amount of reading or discussion can prepare you for the experience of resuscitating a crashing patient. These experiences, real and simulated, are overwhelming and scary, even with flawless knowledge and a skilled team.”
No one who has been there will question the words of Dr. Kaitlin Stockton, a recent graduate of St. Paul’s Emergency Medicine Residency Program, who is one of many young doctors to voice their support for medical simulation training.
“Simulations let us practice as a team in a stressful, fast-paced environment,” says Dr. Stockton. “As a result, you are calmer and more organized in real life scenarios. My simulation experience has helped me overcome real anxiety about leading resuscitations and I’m better prepared for practice because of it.”
Dr. Stockton’s views are echoed by St. Paul’s anesthesiologist Dr. Trina Montemurro, who has participated in simulations with “SimMom,” a high-tech mannequin used to train care teams to deal with a “Code Pink,” which is an emergency in obstetrics.
Dr. Montemurro says up to 11 care team members may be involved in a Code Pink simulation, including a pediatrician and an obstetrician as well as nurses from the OR, maternity and pediatrics, all of who have a job to do and little time to do it.
“Simulations feel very real,” says Dr. Montemurro, “and when you make a mistake in a situation like this, there’s a very good chance you won’t make that mistake again.”
Unified program today will create blueprint for new St. Paul’s Hospital
Simulation programs are not new to St. Paul’s. Along with Maternity and Anesthesiology, who partner on the SimMom program (Maternity also has a neonatal resuscitation simulation program), the Emergency Department has a simulation program as do the ICU and the provincial Heart Centre at St. Paul’s.
What’s new is a plan for a unified Simulation Program, a single program that will serve all of PHC (its hospitals as well as residential care homes) and one that will involve even more departments and divisions beyond those that have programs now.
Currently, physicians at St. Paul’s will often start, and usually help fund, their own simulation programs, which speaks to how strongly care teams believe in simulation as education.
St. Paul’s Foundation has joined this effort to start a unified Simulation Program, making medical simulation an official priority and setting a fundraising goal of $650,000 to help the principal physicians involved get a program started.
One of those physicians is Dr. Jeanne MacLeod, an emergency physician and director of simulation for the St. Paul’s Teck Emergency Centre. Dr. MacLeod is leading the unified Simulation Program effort with Dr. Laine Bosma, who directs the Department of Anesthesiology’s simulation program.
Dr. MacLeod has also collaborated with Dr. Brian Grunau, an emergency physician and director of the Emergency Department extracorporeal cardiopulmonary resuscitation (ECPR) program, which is designed to treat patients who are unable to be revived after a cardiac arrest—a program for which simulation has played a critical role in increasing the experience of hospital staff.
When speaking of a unified program, Dr. MacLeod says she can feel the excitement in the air, especially with the new St. Paul’s Hospital on the horizon.
“Everyone is thinking about the new St. Paul’s Hospital,” says Dr. MacLeod, “so there’s growing interest in the opportunity to have a devoted Simulation Program on the new St. Paul’s Hospital health campus.”
Yet in speaking to the new St. Paul’s Hospital, Dr. MacLeod says just as quickly that the future, as she sees it, is all about the now.
“To look to this future, we need to look at the present, at what we can do today. We need to plant the seeds now. Taking advantage of opportunities today places us in a great position to be leaders in this field at the new St. Paul’s Hospital. That’s very exciting.”
A universal language
Those who have participated in a medical simulation always appreciate the role it plays in communication, and how a simulation helps caregivers from different disciplines communicate with each other more clearly, and so work together more effectively. In a real emergency, there is a handing over of responsibilities and duties, from person to person to person, and it happens very fast. Communication is everything.
“An emergency is one of those times,” says Dr. MacLeod, “when you will have people from different disciplines working together, side by side. When problems occur, they usually occur not because of lack of knowledge but because of lack of communication. We need to know how to communicate with each other and simulations present an opportunity to do that.”
The next generation
It becomes clear very quickly that our younger generation of physicians, many of whom have had the benefit of simulation training from early in their education, tend to be its most vocal champions.
“There is no other training method that comes closer to preparing us for the real thing,” says Dr. Sarah Stonehocker, a recent graduate of the Emergency Medicine program who has participated in several simulations. “A team needs to be able to work together under high-stress conditions. It’s absolutely necessary to be prepared for these kinds of situations, and simulation provides this kind of training benefit.”
Dr. Luke Armstrong, an Emergency physician at St. Paul’s who recently completed his residency, says that simulation sessions were a highlight of his training, and that a simulation program should be a part of any quality training program. Dr. Armstrong doesn’t just mention the education benefits for students, he also points out that simulations allow experienced medical staff to sharpen their skills or learn new techniques.
“Despite how busy Emergency can be,” says Dr. Armstrong, “we can go long periods without seeing particular diseases or trauma. Simulation training not only helps us prepare for specific illness patterns, but also helps develop a safe approach to all patients. Simulations teach you to work as a team, to communicate, and to understand the importance of the role everyone has to play. In any crisis situation, all of these fundamentals are critical.”
The importance of teamwork
There is no question that Dr. Jeanne MacLeod understands what’s involved in starting a PHC-wide simulation training program. This is evident from the ease with which she switches from the smaller, more behind-the-scenes aspects of such a program like maintaining equipment (the “broom closet” side of things, she calls this) to some truly visionary ideas about the very essence of medical education and training that make a unified simulation program sound that much more necessary.
“As students,” says Dr. MacLeod, “so often we study and train individually, yet when we become physicians, we don’t work that way, we don’t work as individuals—we work as part of a team. Yet, we don’t do team training. That team training, such as medical simulation, is a challenge to coordinate because you are coordinating different disciplines and different backgrounds and even different approaches to learning. But when we succeed, when everyone comes together and these exercises happen, the results, as students continue to tell us, can change you. They can be profound.”
Dr. Kaitlin Stockton couldn’t agree more.
“I hope that St. Paul’s Foundation is able to help us start this unified program. It’s important for future trainees as well as for ongoing skill development of current staff, who can maintain the high level of care that’s provided here. It’s so valuable—it’s such a privilege—to work in a hospital that supports this type of teaching.”
You can help our physicians and students create a unified simulation training program by making a gift to St. Paul’s Foundation. We are proud supporters of education initiatives at St. Paul’s and invite you to join us.