This story was told to St. Paul’s Foundation staff member Alexandra Erjavec by Michelle Orr, a nurse and patient educator at the Palliative Care Unit at St. Paul’s Hospital, in February 2023, and is written in Michelle’s words. For confidentiality purposes, we used the pseudonym, “June”.
“Does that mean I’m dying?”
These were the first words June spoke to me after I introduced myself and my role in the Palliative Care Unit at St. Paul’s Hospital. Some patients just stand out, and June was one of them. Everyone deserves to have their story told, and it’s important to me to share June’s story not only to remember her, but also to learn from her to help more patients and their families find peace in the future.
But let me start at the beginning –
June was admitted to St. Paul’s many times throughout her illness over a number of years. Finally, June was admitted in September 2022 after being brought in by ambulance with severe abdominal pain and bleeding. June further suffered a seizure, brain swelling, and a large nose bleed in the hospital and was transferred from Emergency to the Intensive Care Unit (ICU). Her situation was serious and this is when I became involved.
I had read June’s medical history and knew I needed to take a gentle approach when I came in to talk with her. I asked June if it would be ok to get to know her more and to learn about her goals, her story, and where she came from. And that’s where it all took off.
To start, June didn’t want to die.
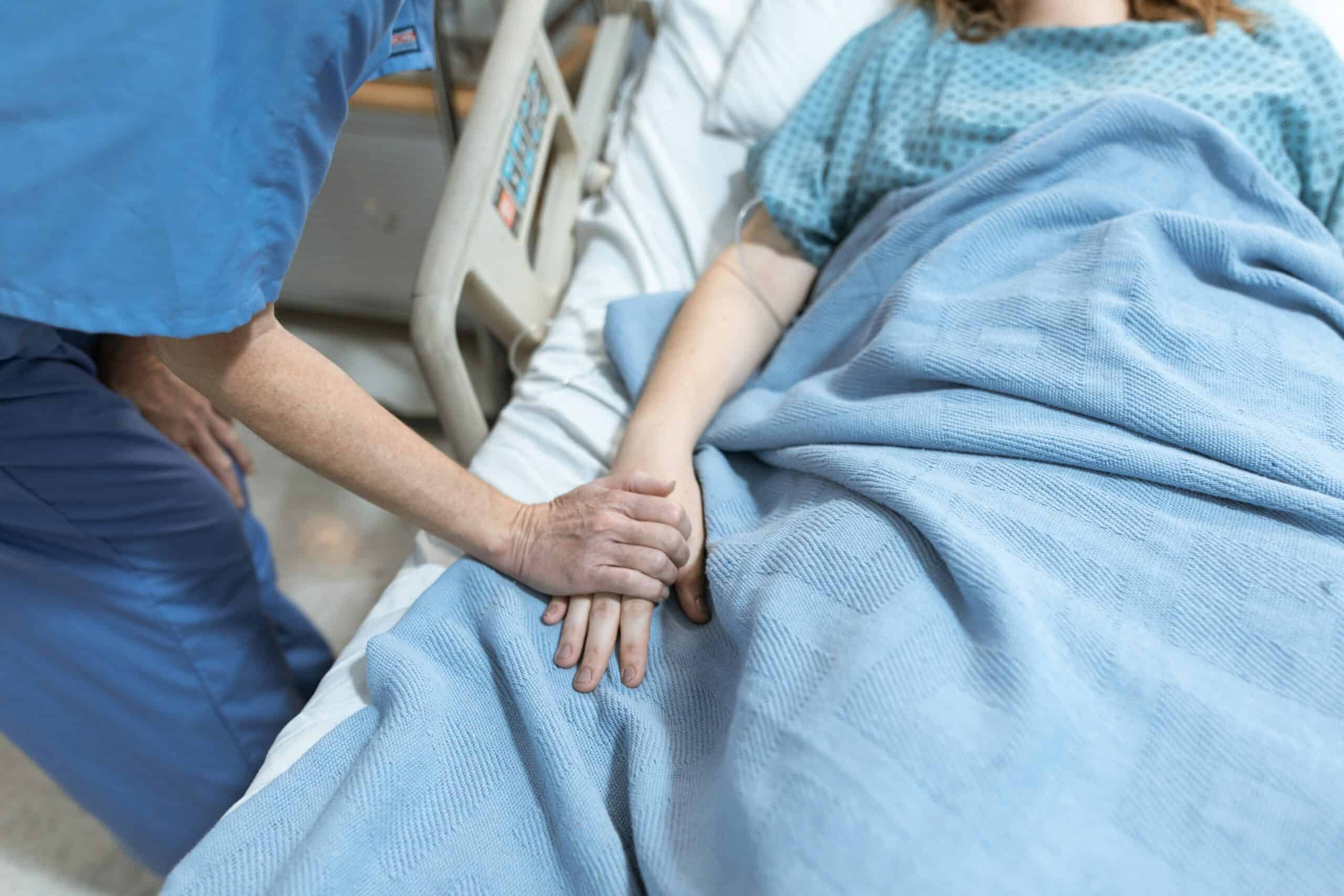
June was very emotional. I would speak with June every day to find out how I could help her and was with her as she went through an extremely painful grief period, made even more painful as she didn’t want any friends or family to know where she was. June expressed feeling lonely and missed being touched – she just wanted someone to hug her and shared that this was one of the hardest things. I couldn’t hug her as we had COVID protocols in place, but I would hold her hand every time we talked.
Over the course of our visits and support from the wider Palliative Care Team, June shifted from feeling that her life was meaningless and a waste, to telling me about her life and how much it meant to her.
June also wanted me to know she was smart (like, really smart), well-educated with a degree from a Canadian university, and worked in a well-paying job. When June brought up that she was previously married and had three kids, the emotional pain of speaking about her children was too great and she couldn’t continue. I could tell that June was experiencing immense grief, pain and suffering. She loved her kids and was incredibly upset that she was no longer part of their life.
The most fragile moment was when June told me about a significant trauma she experienced in her 30s, which then triggered alcoholism. She also told me that this was the first time she had ever told anyone about this traumatic event. It was heartbreaking to hear her talk about her trauma and say, “I never stood a chance. I just couldn’t come back from it.”
Despite speaking with such love for her children and parents, June was adamant that she did not want anyone notified of her location or illness as June had alcohol use disorder, liver cirrhosis (scarring of the liver caused by long-term liver damage), and lived in the Downtown Eastside.
More than anything, June wanted her three kids to know that she loved them, and as a fellow parent, I couldn’t help but feel her pain. We always honour patients’ wishes if they don’t want us to notify anyone, but I just got the feeling that her family loved her and would want to know where she was. I gently probed again for the contact details of her family so that I could share if she passed. She finally agreed and gave me her ex-husband’s phone number.
June died a few weeks later.
I contacted June’s ex-husband and left a couple of voicemails, but he never called me back. I had this uneasy feeling in my stomach because I knew that someone out there loved June and would be upset, and I couldn’t help wishing I had also pushed for her parent’s phone number, even though she didn’t want us to contact them.
Then, a few months later, June’s parents arrived at the Palliative Care Unit at St. Paul’s Hospital.
Turns out, they filed a missing person’s report with Vancouver Police Department when they couldn’t contact June and were notified of their daughter’s death this way, where they also learned that we were the ones to care for her. They loved June so much and had no idea she was so sick. I was afraid they were going to be angry they weren’t notified, but they weren’t. They just wanted to speak with the people who were with June at the end to understand what happened, and to hear June’s story.
I was able to share all the positive things June said about them and her children, their grandchildren. Even though I was still maintaining confidentiality, I could see how much these small stories meant to June’s parents. I broke down and cried when June’s father said, “This will be my grief until the end of my life. I know we weren’t there for her when she needed us, but you were. Thank you.” He looked me in the eyes and touched my hand when he said that.
People who die from addiction aren’t always surrounded by family, and it’s important for the people who are left behind to have a story. So that’s why I wanted to share this – I will always remember June, and telling her story is one of the most meaningful ways I can honour her.